Install the app
How to install the app on iOS
Follow along with the video below to see how to install our site as a web app on your home screen.
Note: This feature may not be available in some browsers.
You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
Koronavirus Suomessa
- Viestiketjun aloittaja AKE-ukki
- Aloitus PVM
Maidan
Respected Leader
Onko se sitten varma että verenohennuslääkkeet auttaa? Entä Primaspan?Itse otan rokotteen heti kun vain saan sen,. Kuulun ns. toiseen riskiryhmään. Ehkäpä Toukokuussa kutsu tulee... saas nähdä!
meidän perheessä on kyllä muunlaisiakin kannanottoja, johtuen tuosta "kohonneesta" tulppariskistä.
Itseäni se ei pelota, koska joudun jo muutenkin syömään veren hyytymisen estolääkkeitä flimmeridiagnoosin vuoksi.
Jos haluat aiheesta toisen mielipiteen, niin voin suositella sitä työpaikkani työterveyden venäläistä naislääkäriä joka hyvin suorasanaisesti sanoi minun olevan vanha ja keskivartalolihava. Sellainen aina lämmittää mieltä eikä pääse ylpistymään suotta..Asiasta on mainittu, mutten ole turhaan tuosta ylpistynyt
AKE-ukki
Respected Leader
Itsekkin olen moista palautetta saanut... Siltä naiselta, joka asuu meidän taloudessa ja väittää olevansa minun vaimoniJos haluat aiheesta toisen mielipiteen, niin voin suositella sitä työpaikkani työterveyden venäläistä naislääkäriä joka hyvin suorasanaisesti sanoi minun olevan vanha ja keskivartalolihava. Sellainen aina lämmittää mieltä eikä pääse ylpistymään suotta..

Fremen
Greatest Leader
Yritän välttää noita työterveyslääkäreitä... viimeksi joku maksoi sellaisen meikäläiselle vissiin vuonna 2007, ja (sattui olemaan naisoletettu) häntä kiinnosti lähinnä kuinka monta alkoholiannosta juon viikossa, ja mikä yleiskuntoni on. Pyysin luvan, ja vedin kaksi leukaa ovenkamanasta (joo menee, jos olet kiipeilijä tasolla 7b+ tai ylemmäs. Kolmas ei kyl olis mennytJos haluat aiheesta toisen mielipiteen, niin voin suositella sitä työpaikkani työterveyden venäläistä naislääkäriä joka hyvin suorasanaisesti sanoi minun olevan vanha ja keskivartalolihava. Sellainen aina lämmittää mieltä eikä pääse ylpistymään suotta..
 ).
).Sen jälkeen olen vältellyt noita. Mutta aikoinaan 1997, kun pääsin Postipankkiin töihin, minulle tehtiin hiv-testi! Ihmettelin jo silloin että oloni ei ole kovin hiv:inen, enkä toivottavasti näytä AIDS-potilaalta, ja miksi vitussa te edes palkkasitte mut jos varma kuolema kolkuttaa porteilla.
Eipä ollut työterveyslääkärillä vastausta. Sanoi noudattavansa saamaansa ohjeistusta.
Ehdotin että elämä voisi olla jännittävämpää jos joskus tekisit päinvastoin.
Emme tavanneet uudestaan.
Hae vaikka naapurista ns toinen mielipide? No ehkä totuuden nimissä on sanottava että ei se lääkäri nyt aivan väärässäkään ollut.. Mutta se slaavilainen töksäytys oli sinänsä huvittava.Itsekkin olen moista palautetta saanut... Siltä naiselta, joka asuu meidän taloudessa ja väittää olevansa minun vaimoni
0,0000004% mahdollisuus veritulppaanSiitä sitten vaan piikkiä käsivarteen ja toivomaan ettei tukosta aivoihin tule. Ei kiitos
vs.
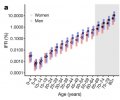
0,05% mahdollisuus kuolla korona infektioon 30-34 vuotiailla miehillä.
Saisinko kaksi rokotetta kiitos? Kumpaankin käsivarteen ja viides vielä perseeseen.
lähde: https://www.nature.com/articles/s41586-020-2918-0/figures/2
Liitteet
vilval
Eversti
Kuulostaa Haaviston hommilta sanotaa notta näin.
Fremen
Greatest Leader
Oookkonää vielä muuten Norjassa? Asia kiinnostaa minua, muistaakseni olit jossain pohjoisessa, jonne ei täältä etelästä ole nyt mitään asiaa. Tosin pääsiäinen tulossa, ja siellä on lunta, ja yritäpä estää norjalaisia tossa tilanteessa... siinä ei fluorivoiteet ja astmasuihkeet ja olympiamitalit paljoa paina, kun täältä lähtee puol miljoonaa suksekasta Tesloillaan pyyhältämään...Kuulostaa Haaviston hommilta sanotaa notta näin.
 .
.Ja niitä ei havut,perkele, paljoa pidättele.
Mitä sitä selvää asiaa kiertelemäänJos haluat aiheesta toisen mielipiteen, niin voin suositella sitä työpaikkani työterveyden venäläistä naislääkäriä joka hyvin suorasanaisesti sanoi minun olevan vanha ja keskivartalolihava. Sellainen aina lämmittää mieltä eikä pääse ylpistymään suotta..

How long might immunity to the coronavirus last? Years, maybe even decades, according to a new study — the most hopeful answer yet to a question that has shadowed plans for widespread vaccination.
Eight months after infection, most people who have recovered still have enough immune cells to fend off the virus and prevent illness, the new data show. A slow rate of decline in the short term suggests, happily, that these cells may persist in the body for a very, very long time to come.
The research, published online, has not been peer-reviewed nor published in a scientific journal. But it is the most comprehensive and long-ranging study of immune memory to the coronavirus to date.
“That amount of memory would likely prevent the vast majority of people from getting hospitalized disease, severe disease, for many years,” said Shane Crotty, a virologist at the La Jolla Institute of Immunology who co-led the new study.
The findings are likely to come as a relief to experts worried that immunity to the virus might be short-lived, and that vaccines might have to be administered repeatedly to keep the pandemic under control.
these studies “are all by and large painting the same picture, which is that once you get past those first few critical weeks, the rest of the response looks pretty conventional,” said Deepta Bhattacharya, an immunologist at the University of Arizona.
Akiko Iwasaki, an immunologist at Yale University, said she was not surprised that the body mounts a long-lasting response because “that’s what is supposed to happen.” Still, she was heartened by the research: “This is exciting news.”
A small number of infected people in the new study did not have long-lasting immunity after recovery, perhaps because of differences in the amounts of coronavirus they were exposed to. But vaccines can overcome that individual variability, said Jennifer Gommerman, an immunologist at the University of Toronto.
“That will help in focusing the response, so you don’t get the same kind of heterogeneity that you would see in an infected population,” she said.

A patient recovering from SARS in China in 2003. Survivors of that infection, also caused by a coronavirus, still carried immune cells 17 years later.Credit...Agence France-Presse — Getty Images
In recent months, reports of waning antibody levels have created worry that immunity to the coronavirus may disappear in a few months, leaving people vulnerable to the virus again.
The Coronavirus Outbreak ›
March 19, 2021, 8:12 p.m. ETMarch 19, 2021
March 19, 2021
But many immunologists have noted that it is natural for antibody levels to drop. Besides, antibodies are just one arm of the immune system.
Although antibodies in the blood are needed to block the virus and forestall a second infection — a condition known as sterilizing immunity — immune cells that “remember” the virus more often are responsible for preventing serious illness.
“Sterilizing immunity doesn’t happen very often — that is not the norm,” said Alessandro Sette, an immunologist at the La Jolla Institute of Immunology and co-leader of the study.
More often, people become infected a second time with a particular pathogen, and the immune system recognizes the invader and quickly extinguishes the infection. The coronavirus in particular is slow to do harm, giving the immune system plenty of time to kick into gear.
“It may be terminated fast enough that not only are you not experiencing any symptoms but you are not infectious,” Dr. Sette said.
Dr. Sette and his colleagues recruited 185 men and women, aged 19 to 81, who had recovered from Covid-19. The majority had mild symptoms not requiring hospitalization; most provided just one blood sample, but 38 provided multiple samples over many months.
TIMES EVENT
On March 23, join Times reporters, Gov. Larry Hogan and others for a subscriber-only event to reflect on one year of the pandemic, and how we come back.
The team tracked four components of the immune system: antibodies, B cells that make more antibodies as needed; and two types of T cells that kill other infected cells. The idea was to build a picture of the immune response over time by looking at its constituents.
“If you just look at only one, you can really be missing the full picture,” Dr. Crotty said.
He and his colleagues found that antibodies were durable, with modest declines at six to eight months after infection, although there was a 200-fold difference in the levels among the participants. T cells showed only a slight, slow decay in the body, while B cells grew in number — an unexpected finding the researchers can’t quite explain.
The study is the first to chart the immune response to a virus in such granular detail, experts said. “For sure, we have no priors here,” Dr. Gommerman said. “We’re learning, I think for the first time, about some of the dynamics of these populations through time.”
Worries over how long immunity to the coronavirus persists were sparked mainly by research into those viruses causing common colds. One frequently cited study, led by Jeffrey Shaman of Columbia University, suggested that immunity might fade quickly and that reinfections could occur within a year.
“What we need to be very mindful of is whether or not reinfection is going to be a concern,” Dr. Shaman said. “And so seeing evidence that we have this kind of persistent, robust response, at least to these time scales, is very encouraging.” So far, at least, he noted, reinfections with the coronavirus seem to be rare.
Exactly how long immunity lasts is hard to predict, because scientists don’t yet know what levels of various immune cells are needed to protect from the virus. But studies so far have suggested that even small numbers of antibodies or T and B cells may be enough to shield those who have recovered.
The participants in the study have been making those cells in robust amounts — so far. “There’s no sign that memory cells are suddenly going to plummet, which would be kind of unusual,” Dr. Iwasaki said. “Usually, there’s a slow decay over years.”
There is some emerging evidence that reinfections with common cold coronaviruses are a result of viral genetic variations, Dr. Bhattacharya noted, and so those concerns may not be relevant to the new coronavirus.
“I don’t think it’s an unreasonable prediction to think that these immune memory components would last for years,” he said.
Eight months after infection, most people who have recovered still have enough immune cells to fend off the virus and prevent illness, the new data show. A slow rate of decline in the short term suggests, happily, that these cells may persist in the body for a very, very long time to come.
The research, published online, has not been peer-reviewed nor published in a scientific journal. But it is the most comprehensive and long-ranging study of immune memory to the coronavirus to date.
“That amount of memory would likely prevent the vast majority of people from getting hospitalized disease, severe disease, for many years,” said Shane Crotty, a virologist at the La Jolla Institute of Immunology who co-led the new study.
The findings are likely to come as a relief to experts worried that immunity to the virus might be short-lived, and that vaccines might have to be administered repeatedly to keep the pandemic under control.
these studies “are all by and large painting the same picture, which is that once you get past those first few critical weeks, the rest of the response looks pretty conventional,” said Deepta Bhattacharya, an immunologist at the University of Arizona.
Akiko Iwasaki, an immunologist at Yale University, said she was not surprised that the body mounts a long-lasting response because “that’s what is supposed to happen.” Still, she was heartened by the research: “This is exciting news.”
A small number of infected people in the new study did not have long-lasting immunity after recovery, perhaps because of differences in the amounts of coronavirus they were exposed to. But vaccines can overcome that individual variability, said Jennifer Gommerman, an immunologist at the University of Toronto.
“That will help in focusing the response, so you don’t get the same kind of heterogeneity that you would see in an infected population,” she said.

A patient recovering from SARS in China in 2003. Survivors of that infection, also caused by a coronavirus, still carried immune cells 17 years later.Credit...Agence France-Presse — Getty Images
In recent months, reports of waning antibody levels have created worry that immunity to the coronavirus may disappear in a few months, leaving people vulnerable to the virus again.
The Coronavirus Outbreak ›
Latest Updates
UpdatedMarch 19, 2021, 8:12 p.m. ETMarch 19, 2021
March 19, 2021
But many immunologists have noted that it is natural for antibody levels to drop. Besides, antibodies are just one arm of the immune system.
Although antibodies in the blood are needed to block the virus and forestall a second infection — a condition known as sterilizing immunity — immune cells that “remember” the virus more often are responsible for preventing serious illness.
“Sterilizing immunity doesn’t happen very often — that is not the norm,” said Alessandro Sette, an immunologist at the La Jolla Institute of Immunology and co-leader of the study.
More often, people become infected a second time with a particular pathogen, and the immune system recognizes the invader and quickly extinguishes the infection. The coronavirus in particular is slow to do harm, giving the immune system plenty of time to kick into gear.
“It may be terminated fast enough that not only are you not experiencing any symptoms but you are not infectious,” Dr. Sette said.
Dr. Sette and his colleagues recruited 185 men and women, aged 19 to 81, who had recovered from Covid-19. The majority had mild symptoms not requiring hospitalization; most provided just one blood sample, but 38 provided multiple samples over many months.
TIMES EVENT
On March 23, join Times reporters, Gov. Larry Hogan and others for a subscriber-only event to reflect on one year of the pandemic, and how we come back.
The team tracked four components of the immune system: antibodies, B cells that make more antibodies as needed; and two types of T cells that kill other infected cells. The idea was to build a picture of the immune response over time by looking at its constituents.
“If you just look at only one, you can really be missing the full picture,” Dr. Crotty said.
He and his colleagues found that antibodies were durable, with modest declines at six to eight months after infection, although there was a 200-fold difference in the levels among the participants. T cells showed only a slight, slow decay in the body, while B cells grew in number — an unexpected finding the researchers can’t quite explain.
The study is the first to chart the immune response to a virus in such granular detail, experts said. “For sure, we have no priors here,” Dr. Gommerman said. “We’re learning, I think for the first time, about some of the dynamics of these populations through time.”
Worries over how long immunity to the coronavirus persists were sparked mainly by research into those viruses causing common colds. One frequently cited study, led by Jeffrey Shaman of Columbia University, suggested that immunity might fade quickly and that reinfections could occur within a year.
“What we need to be very mindful of is whether or not reinfection is going to be a concern,” Dr. Shaman said. “And so seeing evidence that we have this kind of persistent, robust response, at least to these time scales, is very encouraging.” So far, at least, he noted, reinfections with the coronavirus seem to be rare.
Exactly how long immunity lasts is hard to predict, because scientists don’t yet know what levels of various immune cells are needed to protect from the virus. But studies so far have suggested that even small numbers of antibodies or T and B cells may be enough to shield those who have recovered.
The participants in the study have been making those cells in robust amounts — so far. “There’s no sign that memory cells are suddenly going to plummet, which would be kind of unusual,” Dr. Iwasaki said. “Usually, there’s a slow decay over years.”
There is some emerging evidence that reinfections with common cold coronaviruses are a result of viral genetic variations, Dr. Bhattacharya noted, and so those concerns may not be relevant to the new coronavirus.
“I don’t think it’s an unreasonable prediction to think that these immune memory components would last for years,” he said.
vilval
Eversti
Notta en ole Norjassa ollunna mutta verenkierto on viikingeiltä..Tyyryttikö vastaus uteluun?Oookkonää vielä muuten Norjassa? Asia kiinnostaa minua, muistaakseni olit jossain pohjoisessa, jonne ei täältä etelästä ole nyt mitään asiaa. Tosin pääsiäinen tulossa, ja siellä on lunta, ja yritäpä estää norjalaisia tossa tilanteessa... siinä ei fluorivoiteet ja astmasuihkeet ja olympiamitalit paljoa paina, kun täältä lähtee puol miljoonaa suksekasta Tesloillaan pyyhältämään....
Ja niitä ei havut,perkele, paljoa pidättele.
Fremen
Greatest Leader
No emmää tässä mitää udellu... luulin et oot täällä rannikolla? Nou hätä.Notta en ole Norjassa ollunna mutta verenkierto on viikingeiltä..Tyyryttikö vastaus uteluun?
D
Deleted member 1079
Guest
Millainen mahdollisuus kestoerektioon0,0000004% mahdollisuus veritulppaan
vs.
0,05% mahdollisuus kuolla korona infektioon 30-34 vuotiailla miehillä.
Saisinko kaksi rokotetta kiitos? Kumpaankin käsivarteen ja viides vielä perseeseen.
lähde: https://www.nature.com/articles/s41586-020-2918-0/figures/2


Kiinnostaa kiinnostaa...


Fremen
Greatest Leader
Sain/ otin influenssa-rokotteen 2008... ja tulin aika sairaaksi, mutta täytyy sanoa että siihen loppui lentsut, tähän päivään saakka... jotain pientä ollut, mutta ne kausittaiset nuhakuumeet, lihas- ja nivelkipuineen.How long might immunity to the coronavirus last? Years, maybe even decades, according to a new study — the most hopeful answer yet to a question that has shadowed plans for widespread vaccination.
Eight months after infection, most people who have recovered still have enough immune cells to fend off the virus and prevent illness, the new data show. A slow rate of decline in the short term suggests, happily, that these cells may persist in the body for a very, very long time to come.
The research, published online, has not been peer-reviewed nor published in a scientific journal. But it is the most comprehensive and long-ranging study of immune memory to the coronavirus to date.
“That amount of memory would likely prevent the vast majority of people from getting hospitalized disease, severe disease, for many years,” said Shane Crotty, a virologist at the La Jolla Institute of Immunology who co-led the new study.
The findings are likely to come as a relief to experts worried that immunity to the virus might be short-lived, and that vaccines might have to be administered repeatedly to keep the pandemic under control.
these studies “are all by and large painting the same picture, which is that once you get past those first few critical weeks, the rest of the response looks pretty conventional,” said Deepta Bhattacharya, an immunologist at the University of Arizona.
Akiko Iwasaki, an immunologist at Yale University, said she was not surprised that the body mounts a long-lasting response because “that’s what is supposed to happen.” Still, she was heartened by the research: “This is exciting news.”
A small number of infected people in the new study did not have long-lasting immunity after recovery, perhaps because of differences in the amounts of coronavirus they were exposed to. But vaccines can overcome that individual variability, said Jennifer Gommerman, an immunologist at the University of Toronto.
“That will help in focusing the response, so you don’t get the same kind of heterogeneity that you would see in an infected population,” she said.

A patient recovering from SARS in China in 2003. Survivors of that infection, also caused by a coronavirus, still carried immune cells 17 years later.Credit...Agence France-Presse — Getty Images
In recent months, reports of waning antibody levels have created worry that immunity to the coronavirus may disappear in a few months, leaving people vulnerable to the virus again.
The Coronavirus Outbreak ›
Latest Updates
Updated
March 19, 2021, 8:12 p.m. ETMarch 19, 2021
March 19, 2021
But many immunologists have noted that it is natural for antibody levels to drop. Besides, antibodies are just one arm of the immune system.
Although antibodies in the blood are needed to block the virus and forestall a second infection — a condition known as sterilizing immunity — immune cells that “remember” the virus more often are responsible for preventing serious illness.
“Sterilizing immunity doesn’t happen very often — that is not the norm,” said Alessandro Sette, an immunologist at the La Jolla Institute of Immunology and co-leader of the study.
More often, people become infected a second time with a particular pathogen, and the immune system recognizes the invader and quickly extinguishes the infection. The coronavirus in particular is slow to do harm, giving the immune system plenty of time to kick into gear.
“It may be terminated fast enough that not only are you not experiencing any symptoms but you are not infectious,” Dr. Sette said.
Dr. Sette and his colleagues recruited 185 men and women, aged 19 to 81, who had recovered from Covid-19. The majority had mild symptoms not requiring hospitalization; most provided just one blood sample, but 38 provided multiple samples over many months.
TIMES EVENT
On March 23, join Times reporters, Gov. Larry Hogan and others for a subscriber-only event to reflect on one year of the pandemic, and how we come back.
The team tracked four components of the immune system: antibodies, B cells that make more antibodies as needed; and two types of T cells that kill other infected cells. The idea was to build a picture of the immune response over time by looking at its constituents.
“If you just look at only one, you can really be missing the full picture,” Dr. Crotty said.
He and his colleagues found that antibodies were durable, with modest declines at six to eight months after infection, although there was a 200-fold difference in the levels among the participants. T cells showed only a slight, slow decay in the body, while B cells grew in number — an unexpected finding the researchers can’t quite explain.
The study is the first to chart the immune response to a virus in such granular detail, experts said. “For sure, we have no priors here,” Dr. Gommerman said. “We’re learning, I think for the first time, about some of the dynamics of these populations through time.”
Worries over how long immunity to the coronavirus persists were sparked mainly by research into those viruses causing common colds. One frequently cited study, led by Jeffrey Shaman of Columbia University, suggested that immunity might fade quickly and that reinfections could occur within a year.
“What we need to be very mindful of is whether or not reinfection is going to be a concern,” Dr. Shaman said. “And so seeing evidence that we have this kind of persistent, robust response, at least to these time scales, is very encouraging.” So far, at least, he noted, reinfections with the coronavirus seem to be rare.
Exactly how long immunity lasts is hard to predict, because scientists don’t yet know what levels of various immune cells are needed to protect from the virus. But studies so far have suggested that even small numbers of antibodies or T and B cells may be enough to shield those who have recovered.
The participants in the study have been making those cells in robust amounts — so far. “There’s no sign that memory cells are suddenly going to plummet, which would be kind of unusual,” Dr. Iwasaki said. “Usually, there’s a slow decay over years.”
There is some emerging evidence that reinfections with common cold coronaviruses are a result of viral genetic variations, Dr. Bhattacharya noted, and so those concerns may not be relevant to the new coronavirus.
“I don’t think it’s an unreasonable prediction to think that these immune memory components would last for years,” he said.
Poissa.
Jaa-a. On kai niitä helpompiakin keinoja se saada.Millainen mahdollisuus kestoerektioon
Kiinnostaa kiinnostaa...

kimmo.j
Greatest Leader
100% varmuutta ei ole, ikinä, ei minkään lääkkeen kanssa. Kaikissa lääkkeissä on riskinsä.Onko se sitten varma että verenohennuslääkkeet auttaa? Entä Primaspan?
Primaspan auttaa yleisellä tasolla, mutta onko normi annoksesta apua on toinen asia. Ja toisaalta se saattaa aiheuttaa muita ongelmia. Jos taas nostat annosta, kasvatat riskiä saada ongelmia lääkkeestä jolla hoidat ongelmaa.
Siksi lääkärin koulutustus on pitkä, koska ongelmat ovat moni mutkaisia ja vaativat osaamista jota ei löydä netistä.
The Wall Street Journal kertoo, että eurooppalaiset tutkijat ovat löytäneet syyn sille, miksi AstraZenecan koronarokote voi käynnistää joillakin ihmisillä aivolaskimotukoksen rokottamisen jälkeen. Lehti kertoo, että samalla on löydetty myös keinot näiden tapausten hoitoon.
Lehden mukaan kaksi tutkimusryhmää teki itsenäisesti eli toisistaan riippumatta saman havainnon, että rokote voi laukaista autoimmuunireaktion, joka saa veren hyytymään aivoissa. Toinen tutkimusryhmä teki havainnon Norjassa ja toinen Saksassa.
Autoimmuunireaktio tarkoittaa sitä, että ihmisen elimistön immuunijärjestelmä hyökkää kehon omia soluja vastaan.
Norjassa Oslon yliopistollisen sairaalan Pål André Holme sanoo lehden mukaan, että hänen ryhmänsä tunnisti rokotteen luoman vasta-aineen, joka laukaisi haittavaikutuksen.
Saksassa Greifswaldin yliopiston professori Andreas Greinacherin johtama tutkimusryhmä päätyi samaan tulokseen.
AstraZenecan koronarokotteen aiheuttamaa laskimotukosta tutkittiin myös Itävallassa, Irlannissa ja Britanniassa. Saksalaisen tutkijaryhmän mukaan nyt voidaan tunnistaa ne potilaat, joita aivolaskimotukos voi uhata rokottamisen jälkeen. Näillä potilailla ilmeni noin neljä päivää rokottamisen jälkeen samantapaisia oireita eli päänsärkyä, huimausta ja näön heikkenemistä.
– Nyt heidän oireensa aiheuttama vasta-aine voidaan tunnistaa verikokeilla. Tämä tarkoittaa sitä, että AstraZenecan rokotetta ei tarvitse enää pelätä, Greinacher sanoi lehdelle.
– Vain hyvin harvoille ihmisille syntyy tämä komplikaatio, mutta jos näin käy, voimme nyt hoitaa näitä potilaita, hän kertoi.
Rokote laukaisee autoimmuunireaktion
Lehden mukaan kaksi tutkimusryhmää teki itsenäisesti eli toisistaan riippumatta saman havainnon, että rokote voi laukaista autoimmuunireaktion, joka saa veren hyytymään aivoissa. Toinen tutkimusryhmä teki havainnon Norjassa ja toinen Saksassa.
Autoimmuunireaktio tarkoittaa sitä, että ihmisen elimistön immuunijärjestelmä hyökkää kehon omia soluja vastaan.
Norjassa Oslon yliopistollisen sairaalan Pål André Holme sanoo lehden mukaan, että hänen ryhmänsä tunnisti rokotteen luoman vasta-aineen, joka laukaisi haittavaikutuksen.
Saksassa Greifswaldin yliopiston professori Andreas Greinacherin johtama tutkimusryhmä päätyi samaan tulokseen.
AstraZenecan koronarokotteen aiheuttamaa laskimotukosta tutkittiin myös Itävallassa, Irlannissa ja Britanniassa. Saksalaisen tutkijaryhmän mukaan nyt voidaan tunnistaa ne potilaat, joita aivolaskimotukos voi uhata rokottamisen jälkeen. Näillä potilailla ilmeni noin neljä päivää rokottamisen jälkeen samantapaisia oireita eli päänsärkyä, huimausta ja näön heikkenemistä.
– Nyt heidän oireensa aiheuttama vasta-aine voidaan tunnistaa verikokeilla. Tämä tarkoittaa sitä, että AstraZenecan rokotetta ei tarvitse enää pelätä, Greinacher sanoi lehdelle.
– Vain hyvin harvoille ihmisille syntyy tämä komplikaatio, mutta jos näin käy, voimme nyt hoitaa näitä potilaita, hän kertoi.
Pääasia että jokainen tsäänssi on mahdollisuusMillainen mahdollisuus kestoerektioon
Kiinnostaa kiinnostaa...